
The Importance of Planning Ahead with PPE Purchases
Since the first COVID-19 case was identified, in the state of Washington on January 21st, 2020, the virus has spun out of control. In the process, the pandemic has presented serious questions that beg for answers. Various factors have resulted in the United States’ death toll of over 170,415. The lack of personal protective equipment is one component that needs to be resolved quickly or the results will only worsen the significantly high positive cases and death toll.
A new in-depth investigation conducted by the Guardian and Kaiser Health News (KHN) sheds light on the dire circumstances faced by
frontline health workers and their families. Data shows, over nine hundred have lost their lives with the majority being nurses. Their death poses a striking question – did they have to succumb to coronavirus?
Shortage of Personal Protective Equipment (PPE)
The primary purpose of PPE is to protect any employee from health and safety hazards they face at a workplace. For example, viruses like COVID-19 or falling debris at a construction site. However, since the pandemic began, healthcare professionals have protested the massive shortage of it. Many essential workers resorted to wearing bandanas for masks and trash bags for gowns. Even if they did have the necessary equipment, they were forced to reuse it multiple times, thereby increasing their chances of becoming infected.
On April 11th, 2020, Isabelle Papadimitriou, a 64-year-old healthcare worker from Dallas, Texas, messaged her daughter a picture of her three disposable surgical masks she was to reuse. “We don’t have enough PPE,” the text read. Papadimitriou died on July 4th, 2020 due to complications of the virus.
In a separate circumstance, Sarah Roncskevitz, a 32-year-old medical social worker at Kaiser Permanente, an integrated care consortium in San Francisco, lost her battle on May 30th, 2020 after being infected with the virus at her workplace. She was also worried about the shortage of PPE and was concerned that her hospital was unprepared for the pandemic.
A study conducted by the UC Berkeley School of Public Health and UC Berkeley Labor Centre reveals- Out of 607,721 cases in California, at least 50,950 essential workers in the state tested positive as of August 8th, 2020; equalling to 9% of the total case count. The report contends that at least 20,860 workers and associated household COVID-19 cases in California were avoidable if there were enough PPE.
Concerns regarding PPE shortages are heard in various industries outside of workers in medical professions. Essential workers have constantly stated their concern about inadequate health precautions.
The United Food and Commercial Workers Union, a labour union representing 1.3 million workers across America and Canada, is urging to make masks mandatory nationwide and improve their working conditions. As of August 13th, a grim reality has surfaced in their collected data. Reports show there are over 97 grocery worker deaths nationwide, with 7,188 grocery workers infected and at least 6,122 grocery workers highly exposed to COVID-19.
Early Warning Signs Were Ignored
Prior to the pandemic, infectious disease specialists and epidemiologists regularly ran simulations of a possible outbreak. One of these simulations was conducted in 2005 by the federal government and was very similar to what’s happening today; a respiratory virus that started in China and made its way to the rest of the world. The New York Times covered this story and among the various issues found was, ‘Deficiencies in Personal Protective Equipment’. The test found that the US was unable to produce PPE rapidly when required.
Though America has faced the threat of viruses before, the full extent of the possible damage was not felt earlier. In the case of countries such as South Korea and Japan, amongst others, they were well-versed with the severity of a contagious respiratory disease as seen in the SARS outbreak and were prepared for COVID-19. In the US, the least that should have been done was to immediately ramp up the production of PPE once the news of coronavirus was announced in January. The government authorities focused on travel bans which, though useful, did not address the internal problem.
In fact, in the early days of the pandemic, the Department of Health and Human Services clarified that the United States had only 1% of the required respirator masks for medical professionals. They estimated that 3.5 billion N95 masks would be required for one year. However, the nation’s emergency stockpile of drugs and medical supplies, held only approximately 12 million medical-grade N95 respirator masks and 30 million surgical face masks. Even though pharmaceutical companies like 3M and General Electric ramped up production of PPE and ventilators, the damage was done.
Why is the Stockpiling of PPE Important?
The current pandemic left us defenceless, but all is not lost as it serves as a lesson for future events. One of the most crucial factors in deciding the impact of a virus is the presence or the lack of PPE. A shortage of PPE causes the cases to skyrocket by unnecessarily exposing individuals, especially frontline workers who can transmit the disease to their family. With a pandemic like COVID-19, where individuals could be positive but asymptomatic, it is vital to stop the transmission as it is the same people who carry the virus and infect vulnerable members of society. The benefits of stockpiling PPE are numerous and it should become a regular practice in the United States and the rest of the world even after a vaccine is found for COVID-19.
Economic Benefits
PPE prices have increased massively since the start of the pandemic as demand soared drastically. According to the study by the Berkeley Labor Center, New York State, the worst hit state early in the pandemic, paid $7.50 for each high grade N95 mask. The same mask would have cost close to $1, depending on the quality prior to the pandemic. The federal government, through its bulk purchasing power, reportedly placed no-bid contracts at six times the price.
Similarly, on April 7th, California signed a bulk contract with an unproven supplier for 300 million NIOSH approved N95 masks. While the price was set at $5.90 for rapid delivery, they paid significantly lower at $3.30 per mask as the delivery was delayed until June 2020. This left California facing huge setbacks during the first three months of COVID-19.
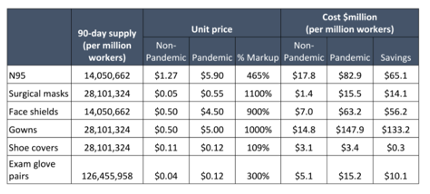
Cost of 90-day supply of PPE per million health workers as investigated by UC Berkeley Labor Center.
Cost of procuring PPE depends on the number of workers, type of workers covered and the timing. Per the price estimates in the table above, procuring real-time PPE during a pandemic would cost over $808 million whereas, if procured during non-pandemic times, it would only cost $134 million; 17% of the cost at pandemic prices.
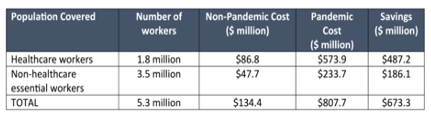
This table looks at PPE costs for healthcare workers and non-healthcare essential workers – Data provided by UC Berkeley Labor Center.
Evidently, investing in PPE would produce massive economic benefits even if used years later.
Unemployment Benefits Due to PPE Shortages
A record number of healthcare workers have lost their jobs due to the pandemic. The US Bureau of Labor Statistics reports that 1.4 million healthcare workers lost jobs in April, out of which 134,900 worked in hospitals. Other individuals included people engaged in ambulatory services, dentists (503,300), physicians (243,300), and other healthcare practitioners (205,100).
Many couldn’t provide services without adequate PPE, which resulted in a loss of livelihood for workers and the lack of necessary access to healthcare for patients. Besides, the state governments have spent millions of dollars supporting those who cannot perform the procedures. If there were sufficient PPE, the workers would have returned earlier and even if it’s just by a week, the money saved would have been enormous.
Will PPE be Required After a Vaccine?
Top pharmaceutical companies around the world such as Pfizer, Moderna and AstraZeneca, among others, are in the race for developing a vaccine. If successful, the vaccine would be a gamechanger. Does this eliminate the need for PPE though?
In an interview, Maria Elena Bottazzi, a microbiologist and the Associate Dean of the National School of Tropical Medicine at Baylor College of Medicine, states, the vaccine will probably reduce, but not completely eliminate the chance of an inoculated person being infected by the coronavirus. The effectiveness of the vaccine needs real-world testing, and that can only happen when it’s in the wild for a significant period. Therefore, life will not immediately return to normal after the vaccine is available for the masses. PPE will still be necessary, and so will the social distancing rules. Slowly, but eventually, life will return to normal.
Supply Chain Logistics
Since March, supply chains have come into national focus. As most of America’s supplies were sourced outside the country, they were under pressure to perform. Businesses have to focus on multiple fronts. At a time like this, and in the future, supply chain management is extremely crucial.
In the U.S., manufacturers repurposed existing production lines or launched new ones. Some figured the demand to last beyond the immediate threat and others wanted to gain “essential” status to keep the machines running, and people working.
In response to COVID-19, there are end-to-end supply chain actions to consider, such as:
- Determining the origin of supply and identifying potential risks along the chain is necessary. The other alternatives for supply and distribution should be considered.
- Assessing the impact on operations and ensuring employee safety, but also optimizing the production and distribution capacity.
- Estimating the available inventory, and having a realistic understanding of the final customer’s demand.
- Secure the capacity of the logistics and improvise.
- Run stress tests to get a better picture of the whole chain.
After immediate risks to the supply chain are identified, the process needs to be scrutinised closely to ensure that various situations are considered with adequate plans to overcome the obstacles.
And Finally…
COVID-19 has impacted the modern world on a large scale. The repercussions of it will last for decades to come, but the lessons gained from it will be key for a quicker recovery. The one learning from it: Plan and stockpile PPE for a better tomorrow.
In partnership with a leading non-profit Behavioral Health Provider, our quality protective gear and safety equipment are of the highest quality meeting global health standards as prescribed by the World Health Organization (WHO), FDA and CE in our manufacturing and delivery cycle to ensure client welfare.
